- World Population Review Newsletter
- Posts
- Where Antibiotics Are Failing—and What Comes Next
Where Antibiotics Are Failing—and What Comes Next
Medical practices driving a silent, global breakdown in treatment.
Greetings, inquisitive mind of global health and human resilience!
One of medicine’s greatest breakthroughs is quietly losing its edge.
Antibiotics still work—until they don’t. And when they fail, the consequences arrive late, expensive, and often irreversible.
Below are seven places where resistance risk is already high—and what their choices reveal about the future of reliable medical care.
You're overpaying for crypto.
Every exchange has different prices for the same crypto. Most people stick with one and pay whatever it costs.
CoW Swap checks them all automatically. Finds the best price. Executes your trade. Takes 30 seconds.
Stop leaving money on the table.
India sits at the center of the global antibiotic resistance challenge—not due to negligence, but scale.
With over 1.4 billion people and uneven access to healthcare, antibiotics are often purchased without prescriptions, used inconsistently, or stopped early when symptoms fade. This creates ideal conditions for resistant bacteria to evolve.
India is also one of the world’s largest producers of generic antibiotics, which improves access globally—but also increases environmental exposure when manufacturing waste enters waterways.
The country has made progress through stewardship programs, yet enforcement remains difficult across vast rural and urban populations.
A sobering data point: India accounts for a significant share of global deaths linked to drug-resistant infections each year, according to international health estimates.

China has dramatically modernized its healthcare system—but antibiotic resistance remains a persistent shadow.
For years, hospital funding structures unintentionally encouraged over-prescription, with antibiotics frequently used as a default treatment. Although reforms have reduced unnecessary prescribing, resistance rates remain elevated in many regions.
China’s massive livestock sector also plays a role. Antibiotics have long been used to promote animal growth, contributing to resistant strains that move from farms to humans.
The country is now investing heavily in surveillance and regulation, but reversing decades of overuse takes time.
Key insight: Some hospital-acquired infections in China now show resistance to multiple last-line antibiotics.

Several Southern European countries face higher resistance rates than their northern neighbors, despite strong healthcare systems.
The drivers are subtle: patient expectations for antibiotics, cultural norms around medication, and inconsistent adherence to treatment guidelines. In some regions, doctors report prescribing antibiotics simply to meet patient demand.
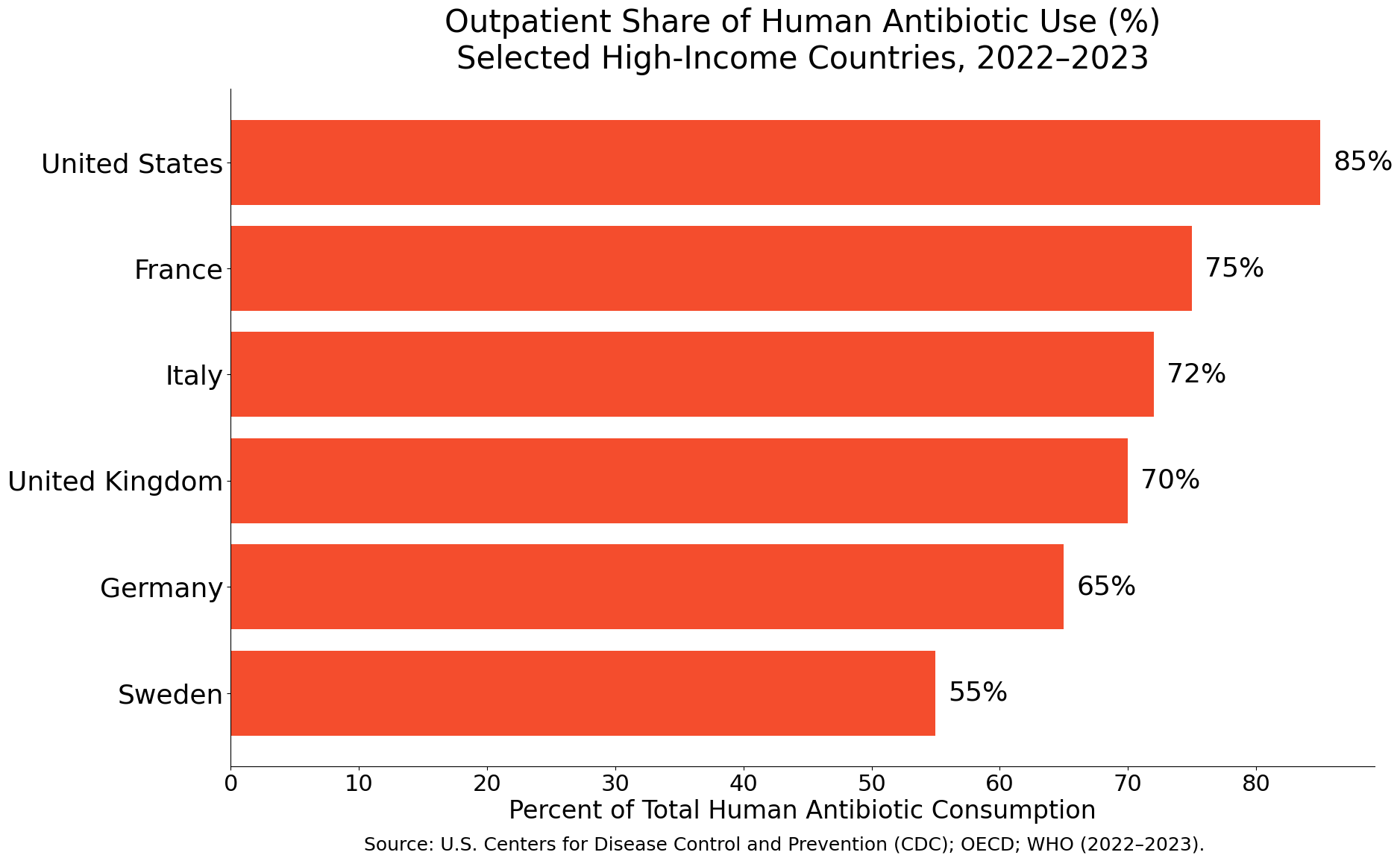
This is compounded by high outpatient antibiotic use—often for viral infections where antibiotics offer no benefit.
Efforts to improve prescribing habits are underway, but progress varies widely by country and region.
Notable contrast: Antibiotic use in parts of Southern Europe is nearly double that of Scandinavian countries.

Learn how to make AI work for you
AI won’t take your job, but a person using AI might. That’s why 2,000,000+ professionals read The Rundown AI – the free newsletter that keeps you updated on the latest AI news and teaches you how to use it in just 5 minutes a day.
The U.S. has world-class hospitals—and a resistance problem hiding in plain sight.
Overprescription in outpatient settings, widespread use in industrial agriculture, and inconsistent stewardship across states all contribute. While hospitals have improved infection control, community-level misuse remains common.
Agricultural antibiotic use is a particular concern, as resistant bacteria can spread through food systems and the environment.
Innovation is strong, but coordination is not always.
A critical warning: Some common infections in the U.S. are now resistant to three or more antibiotic classes.
Southeast Asia has become a hotspot for antibiotic resistance due to rapid urbanization, dense populations, and heavy antibiotic availability.
In many countries, antibiotics are easily purchased over the counter. Combined with high tourism and global trade, resistant strains travel quickly across borders.
Healthcare infrastructure varies widely—from world-class private hospitals to under-resourced rural clinics—making uniform policy enforcement difficult.
The region is now a focal point for global monitoring efforts.
Quiet reality: International travelers can carry resistant bacteria home without ever knowing it.

In parts of Sub-Saharan Africa, the challenge isn’t excess—it’s imbalance.
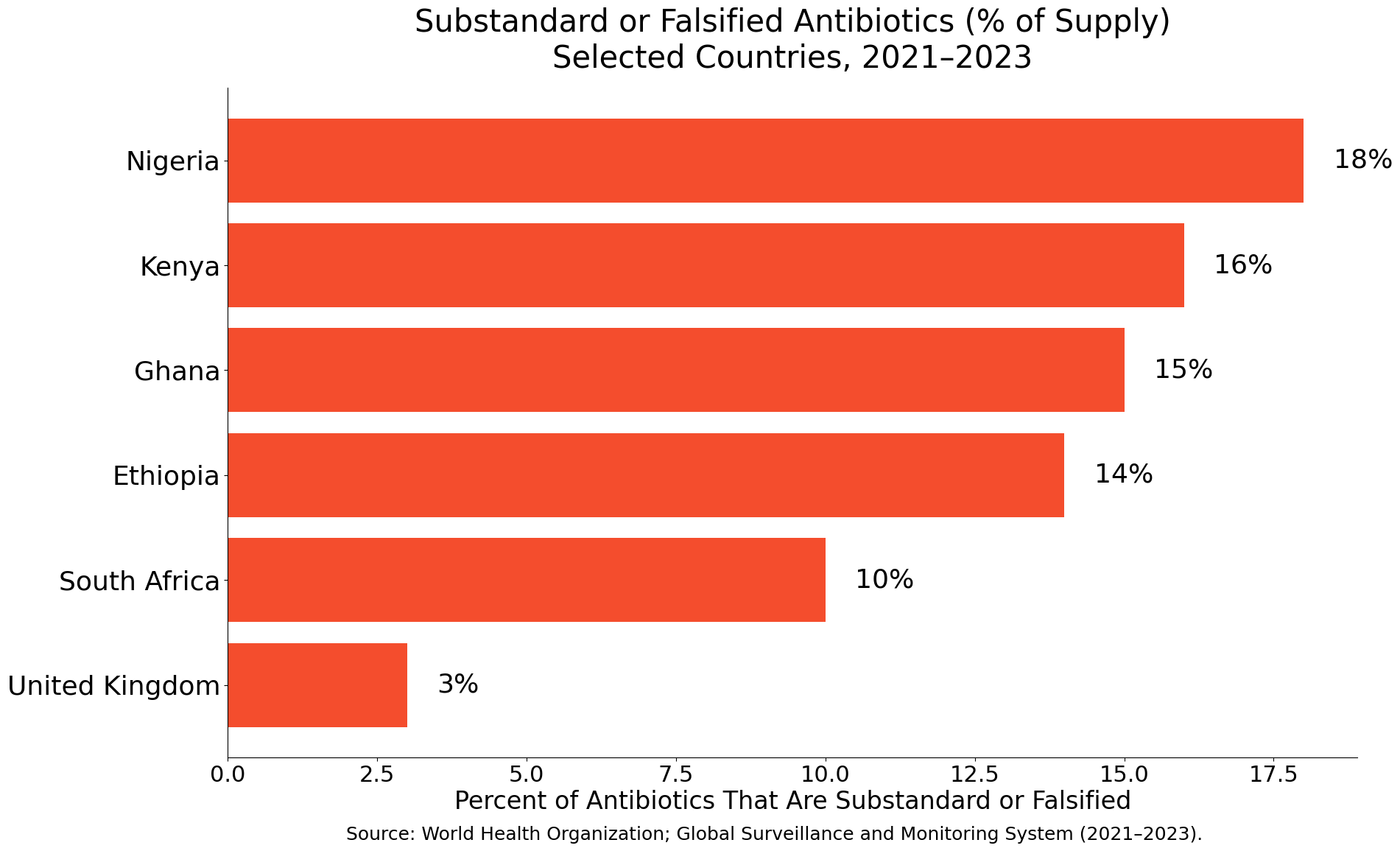
Limited access to diagnostics means antibiotics are often used “just in case.” Counterfeit or substandard drugs further accelerate resistance by exposing bacteria to ineffective doses.
At the same time, lack of clean water and sanitation increases infection rates, driving higher antibiotic demand in the first place.
The result is a feedback loop that’s hard to break without systemic investment.
Hard truth: Some resistant infections in the region now have mortality rates comparable to untreated diseases of the pre-antibiotic era.
Scandinavia offers a powerful counterexample.
Countries like Sweden and Norway enforce strict antibiotic prescribing rules, limit agricultural use, and invest heavily in public education. Patients expect restraint, not prescriptions.
The result is some of the lowest resistance rates in the world—and antibiotics that still work when truly needed.
This shows that resistance is a policy and cultural outcome, not an unavoidable fate.
Encouraging fact: Scandinavian antibiotic consumption per capita is among the lowest globally—and outcomes are better, not worse.

Antibiotic resistance is not a distant threat. It’s already reshaping healthcare quality, surgical safety, and long-term health outcomes—especially for older populations.
For anyone considering where to live, retire, or seek medical care, resistance rates matter as much as hospital rankings or insurance systems.
The countries that protect antibiotics today will offer safer medicine tomorrow.
Stay informed. Stay proactive. And keep exploring the forces shaping global health beneath the surface.
Warm regards,
Shane Fulmer
Founder, WorldPopulationReview.com
P.S. Want to sponsor this newsletter? Reach 148,000+ global-minded readers — click here!


